Healthcare systems cannot cut their way out of the current cost crisis. Medical costs rose 7.5–8.5% in 2024 and are projected to stay at that rate through 2026. Health system EBITDAs have dropped 11% since 2019. The answer is Intelligent Business Transformation, a structural overhaul of how healthcare organisations are designed, how decisions get made, and how technology eliminates the operational drag costing systems millions every quarter.
The Data Behind the Crisis
Margin compression from macroeconomic headwinds alone could push operating costs up by more than 1,500 basis points. Yet the more alarming statistic is internal: 81% of C-suite health system leaders say their current operating model is not effective or efficient and 48% have already attempted a redesign in the last two years that hasn’t delivered.
Most redesigns fail because they address symptoms, a new EHR, a cost reduction programme, a restructured org chart, without fixing the structural causes underneath.
The structural cause is operational friction: disconnected systems, decisions made by committee, and talent deployed against the wrong priorities.
The Three Pillars of Intelligent Business Transformation in Healthcare
Pillar 1 : Organisational Structure – Build a Federated Model
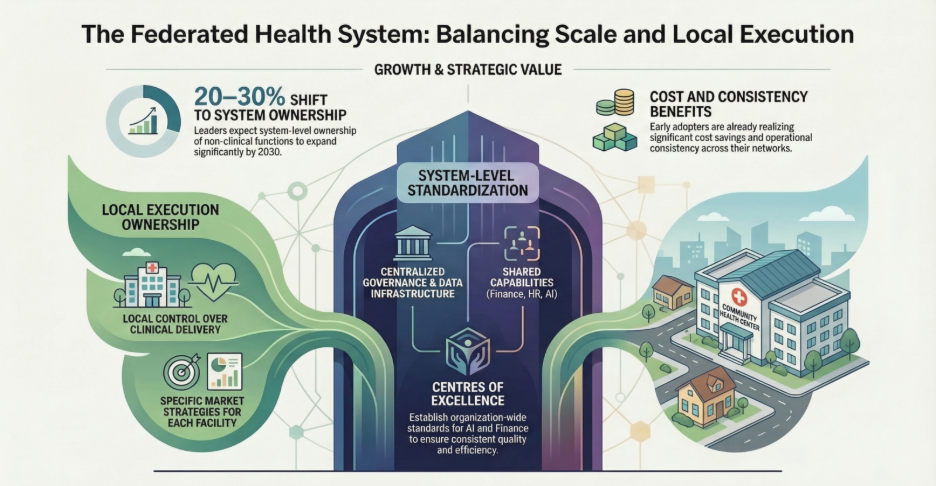
The question is not centralise vs. decentralise. It is: what should be standardised at the system level, and what should remain locally executed?
Leading health systems are moving to a federated architecture, centralising governance, data infrastructure, and shared capabilities while preserving local execution for clinical delivery and market strategy. Systems implementing this model are building Centres of Excellence for AI, finance, and HR that set organisation-wide standards, while facility teams retain day-to-day ownership.
Survey data shows leaders expect the share of nonclinical functions owned at system level to expand by 20–30% over the next three to five years. The systems moving early are already realising the cost and consistency benefits of that shift.
Pillar 2 : Decision Making – Fix the Committee Problem
The single highest-ROI opportunity in healthcare operating model redesign is not a technology investment. It is fixing how decisions get made.
Current benchmarks reveal the scale of the problem:
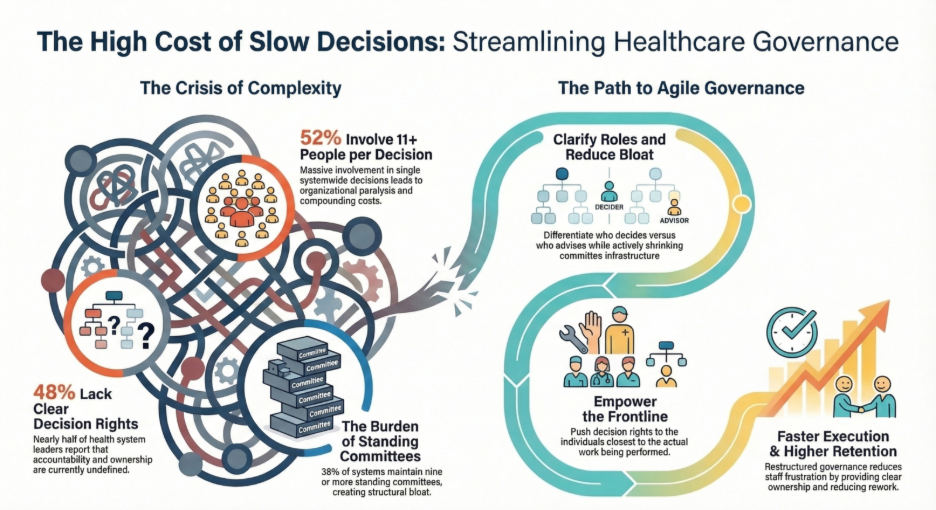
- 52% of health system leaders report 11 or more people involved in a single systemwide decision
- 38% have nine or more standing committees
- 48% say decision rights and accountability are unclear
Every slow decision has a compounding cost, delayed capital approvals, duplicated procurement spend, critical roles sitting vacant for months.
Intelligent Business Transformation addresses this through six targeted changes: clarifying who decides vs. who advises, reducing committee infrastructure, pushing decisions to the person closest to the work, standardising decision language, using real-time data instead of monthly reports, and automating routing for high-volume low-complexity decisions.
Outcome: Health systems that have restructured decision governance report faster execution, reduced rework, and measurably higher staff retention, because clarity of ownership directly reduces organisational frustration.
Pillar 3 : Technology – Platform Engineering as the Enabler
Structural change first. Technology second. But the technology layer is what makes transformation scalable.
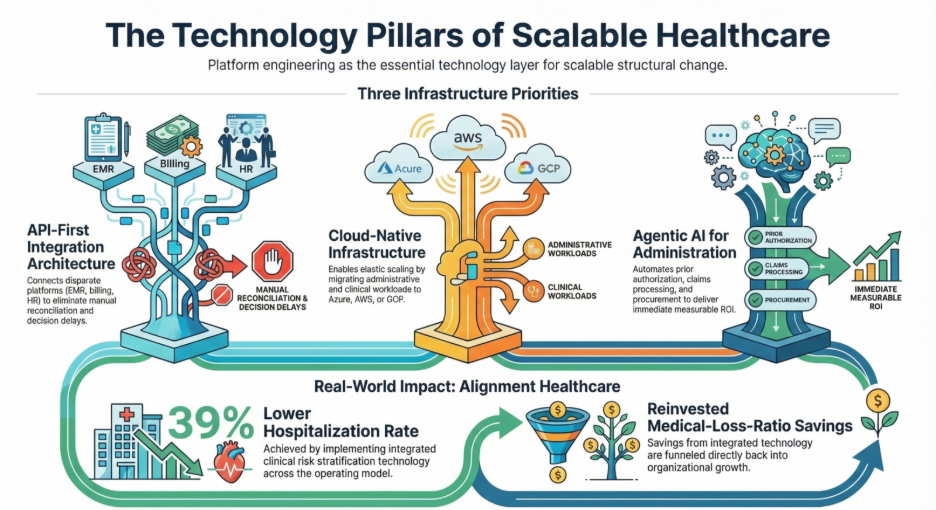
Three infrastructure priorities matter most right now:
API-first integration architecture: Most health systems run 15–30 separate platforms that cannot share data in real time. Building a platform engineering layer that connects EMRs, billing, HR, supply chain, and finance eliminates the manual reconciliation and decision delays that compound into significant annual cost.
Cloud-native infrastructure: Legacy on-premise systems cannot absorb demand spikes without significant capital cost. Migrating to Azure, AWS, or GCP on a phased basis, starting with administrative workloads, then progressing to clinical systems, enables elastic scaling and faster deployment without disrupting operations.
Agentic AI for administrative workflows : The highest-value immediate AI opportunity in healthcare is not clinical. It is administrative. End-to-end automation of prior authorisation, claims processing, procurement replenishment, and revenue cycle management with human review at critical checkpoints is delivering measurable ROI at systems that have deployed it today.
Real-world result: Alignment Healthcare USA implemented integrated clinical risk stratification technology across its operating model. Its hospitalisation rate now runs 39% below Medicare’s rate in its markets, with medical-loss-ratio savings reinvested directly into growth.
How to Start: A Four-Step Roadmap
- Clarify objectives with measurable targets : define cost reduction benchmarks, decision cycle time goals, and retention improvement metrics before beginning
- Build an organisational blueprint : map roles and responsibilities across system, market, and facility levels; identify where blurred accountability is producing duplicated effort
- Redesign two or three high-friction processes immediately : prior authorisation, capital approvals, or procurement replenishment; use these as proof points before scaling
- Invest in leadership development aligned to the new model : AI fluency, data-driven decision-making, and federated ownership mindsets are non-negotiable capabilities for the operating model ahead
Frequently Asked Questions
What is Intelligent Business Transformation in healthcare?
It is the structural redesign of how a healthcare organisation operates, combining organisational redesign, process automation, talent redeployment, and technology integration to eliminate operational friction and build financial resilience against sustained cost inflation.
How does fixing decision-making reduce operating costs?
Slow consensus-driven decisions increase the cost of every operational function. Systems that clarify decision rights and reduce committee infrastructure report faster execution, less rework, and improved staff retention, all with direct cost impact.
How long does healthcare operating model transformation take to show results?
Structural quick wins, decision rights clarification, integration of two or three key systems, process redesign, can deliver measurable results within 90–180 days. Full transformation runs 18–36 months, with value realised progressively at each phase.
Can health systems implement AI without disrupting clinical operations?
Yes. Starting with administrative and back-office workflows, prior authorisation, claims, HR, procurement, delivers immediate ROI with minimal clinical risk. Clinical AI is introduced progressively with human-in-the-loop governance at every stage.
The Bottom Line
The health systems that will be financially viable in 2028 are not the ones that cut hardest in 2025. They are the ones that used this period of pressure to redesign how they operate, connecting systems, empowering faster decisions, and deploying technology where it creates durable value.
200OK Solutions partners with healthcare organisations to deliver Intelligent Business Transformation end to end, from platform engineering and cloud-native infrastructure to intelligent automation and organisational change.
Get in touch to discuss where your operating model needs to go next.
You may also like: Building EU Ready Digital Platforms: A Technical Blueprint for Compliance and Scale


