Healthcare organisations are spending more on workforce training than ever, yet productivity, staff retention, and patient outcomes continue to decline. The real problem is not a skills gap. It is a structural and operational one. Until healthcare leaders address the root causes, fragmented workflows, misaligned incentives, outdated technology, and siloed decision-making, no amount of e-learning or training investment will move the needle.
The Uncomfortable Truth About Healthcare Workforce Productivity
Healthcare CEOs, COOs, and CTOs are under unprecedented pressure. Staffing costs are rising. Burnout is accelerating. And despite significant investment in e-learning for healthcare staff, compliance training, and upskilling programmes, organisations are not seeing proportional gains in performance.
The question every decision-maker should be asking is not “How do we train our people better?”, it is “Why are our trained people still unable to perform at full capacity?”
The answer almost always points to structural and operational failures hiding beneath the surface.
Why Training Alone Is Not Enough: The Root Causes
Here are the structural root causes that training budgets simply cannot fix:
1. Fragmented Technology Infrastructure
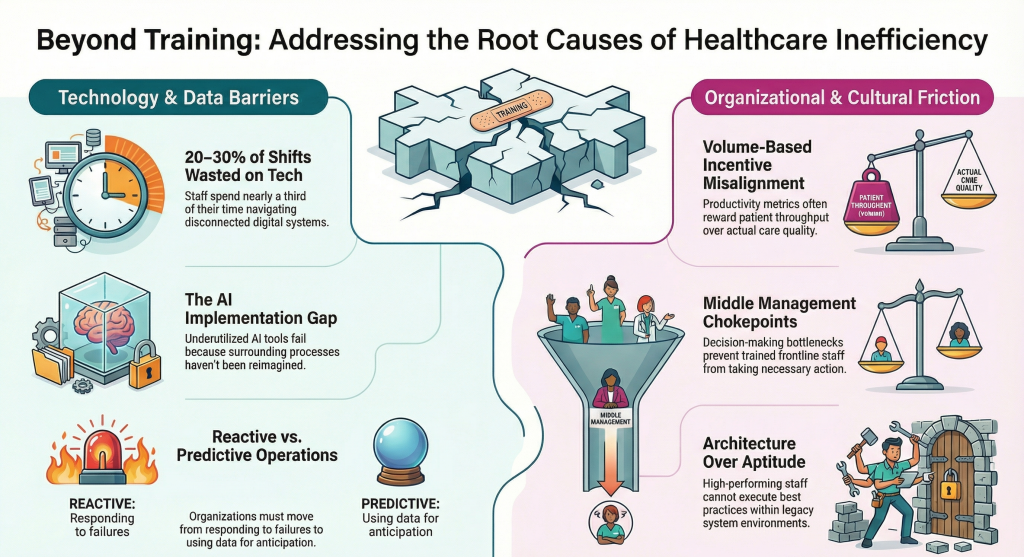
When clinical staff spend 20–30% of their shifts navigating disconnected systems, from patient records to scheduling to compliance tools, no training programme resolves that friction. The problem is architecture, not aptitude.
-
- Staff trained on best-practice workflows cannot execute them in legacy system environments
-
- Disconnected data silos force workarounds that erode efficiency at scale
-
- The promise of AI in healthcare is undermined when the underlying operational layer is broken
2. Misaligned Incentive Structures
Productivity metrics in many healthcare organisations still reward volume over value, patient throughput over care quality. This misalignment means even high-performing, well-trained staff are optimising for the wrong outcomes. Leaders must redesign incentive frameworks before investing further in skills development.
3. Decision-Making Bottlenecks
Middle management layers, often themselves under-resourced, become the operational chokepoint. Frontline staff are trained to act, but lack the authority or information to do so. Intelligent business transformation addresses this directly: it restructures decision rights, not just competencies.
4. Failure to Leverage Digital and AI Capabilities
The gap between what digital healthcare technology can deliver and what organisations actually deploy is enormous. Many healthcare providers have invested in platforms but not in the operational redesign needed to make them work. AI and automation tools remain underutilised not because staff lack training on them, but because the processes around them have not been reimagined.
5. Reactive Rather Than Predictive Operations
Healthcare organisations predominantly operate in reactive mode, responding to workforce shortages, compliance failures, and performance gaps after they occur. An intelligent operational framework shifts this to predictive and preventative: using data to anticipate demand, flag risk, and resource proactively.
How to Diagnose If Your Organisation Has a Structural Problem
Ask your leadership team these questions:
-
- Are trained staff regularly unable to apply what they have learned because of system or process constraints?
-
- Do your performance dashboards show consistent team-level underperformance despite individual competence?
-
- Is your risk management and healthcare policy function primarily reactive?
-
- Has your investment in digital healthcare tools not translated into measurable efficiency gains?
If the answer to two or more is yes, you have a structural problem and a training-first strategy will continue to underdeliver.
What Intelligent Business Transformation Looks Like in Healthcare
At 200OK Solutions, our approach to intelligent business transformation in healthcare does not begin with a training needs analysis. It begins with an operational diagnostic.
We help healthcare leaders:
-
- Map the true cost of structural inefficiency, not headcount or hours, but the downstream impact on patient outcomes, staff retention, and regulatory risk
-
- Redesign workflows with AI and data at the core, embedding intelligence into daily operations, not bolting it on
-
- Align technology investment with operational reality, ensuring your AI and healthcare strategy is grounded in what frontline teams actually need
-
- Build decision-making infrastructure, so that insight reaches the people who need it, at the speed care demands
-
- Create performance frameworks that sustain change, not one-off training events, but systemic capability that compounds over time
This is not about replacing your workforce. It is about removing the structural barriers that prevent your workforce from performing at the level their training has prepared them for.
The Business Case for Acting Now
Healthcare systems globally are under strain. The organisations that will emerge stronger are those that treat workforce productivity as a systems problem, not a people problem.
The ROI is measurable:
-
- Reduced agency and locum spend through better demand forecasting
-
- Lower attrition rates when staff operate in high-functioning environments
-
- Faster regulatory compliance through automated monitoring and reporting
-
- Better patient outcomes tied directly to operational consistency
The Bottom Line
Workforce productivity in healthcare is not primarily a training problem. It is a structural one. Until leaders confront the operational, technological, and governance conditions in which their workforce operates, training spend will continue to deliver diminishing returns.
The organisations that will lead healthcare in the next decade are those that invest in intelligent business transformation, redesigning the systems, not just developing the people within them.
Ready to move beyond training budgets and fix the structural root causes? Explore how 200OK Solutions helps healthcare leaders build operationally intelligent organisations at 200oksolutions.com.
Frequently Asked Questions
Q. How does intelligent business transformation differ from standard healthcare consulting?
A. Traditional healthcare consulting focuses on recommendations and process documentation. Intelligent business transformation is outcome-led: it combines operational redesign, technology integration, and AI-enabled decision support to deliver measurable, sustained change, not slide decks.
Q. What is the first step for a healthcare CEO looking to address workforce productivity?
A. Start with an operational diagnostic, not a training audit. Map where your highest-performing staff are losing time, where decisions are being delayed, and where your digital tools are creating friction rather than reducing it. The answers will reveal whether your productivity problem is structural, technological, or cultural, and what to address first.
Q. How quickly can AI in healthcare deliver productivity gains?
A. Organisations that have redesigned workflows alongside AI deployment, rather than simply adding AI tools to existing processes, typically see measurable efficiency improvements within 6–12 months. The technology is rarely the bottleneck. The constraint is almost always operational readiness.
Can small and mid-sized healthcare providers benefit from intelligent transformation?
Absolutely. Structural inefficiency compounds at any scale. Mid-sized providers often achieve faster results because decision-making is less fragmented and change can be implemented more rapidly.
You may also like: Procurement Consolidation: How Healthcare Finds Margin


